Digital virology pipeline brings AI’s expert eye to identifying infections
Microscopy plus machine learning equals a quick, cheap and automated way to detect not only coronavirus, but other emerging pathogens or cellular responses to drugs.
Image: Minttu Polso
Before there were vaccines or good ways to diagnose SARS-CoV-2, scientists around the world were scrambling to develop methods for understanding the biology of the virus. While the pandemic opened plenty of scientific opportunities and questions, doors and borders were also shut almost everywhere. One of the millions of people who was stuck during early 2020 was computer scientist Christian Guckelsberger. Due to start a postdoc on AI and creativity in Finland, he instead found himself part of an international biomedical research project to harness machine learning to identify the coronavirus from patient blood samples.
“It was like being thrown into cold water. I’m not a medical person and hadn’t thought about these kinds of things since high school biology,” says Guckelsberger, now an assistant professor of creative technologies at Aalto University and FCAI. “But this project gave me the feeling of doing something relevant and putting my mind to best use at a critical time.” Amid pandemic travel restrictions, Guckelsberger’s involvement in the timely, multidisciplinary project allowed him to come to Finland and embark on what he thought would be a two-month project. It ended up lasting an entire year and sparked a renewed fascination for biomedical research and the people doing it.
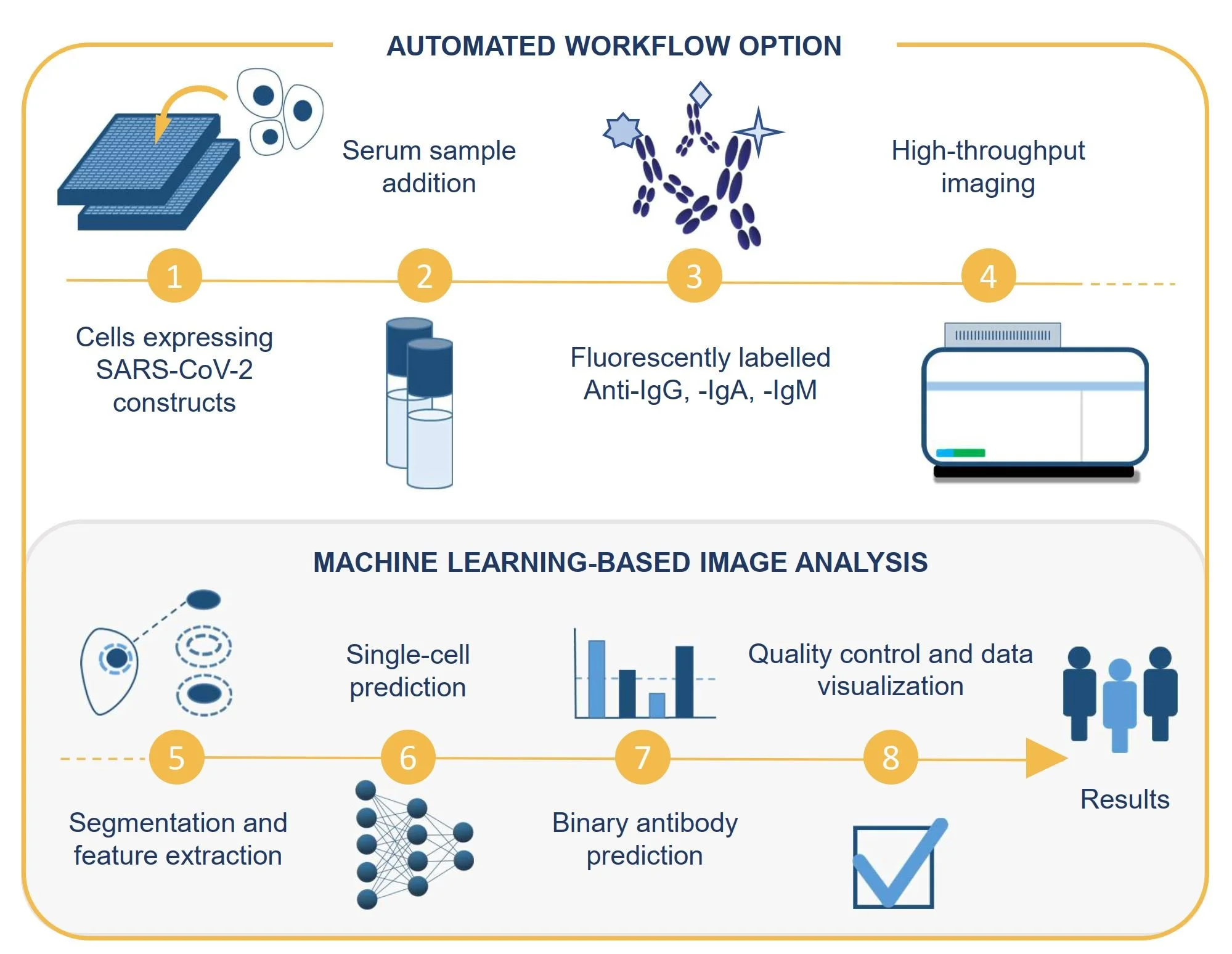
What Guckelsberger and colleagues developed during that year is a way to automatically classify digital microscopy images of the interactions between antibodies and virus antigens in lab-grown cells. A computer essentially learns to detect if the patient has anti-coronavirus antibodies. Beyond a diagnosis, the method also gives researchers insight into what features in cells indicate a positive result, what kind of antibody responses are present and allows them to make predictions about the likelihood of a COVID-19 antibody positive sample from the image alone.
The same sample images classified by a computer were also shown to expert virologists, who rated them as positive or negative for coronavirus antibodies. “Our approach can match the classification level of human experts,” says Guckelsberger, “and it’s much faster. Plus, it can tell us when there are ambiguous results that should be given a closer look by an expert eye.”
The results of the project, recently published in Cell Reports Methods, also show that the method is comparable, and in some ways superior, to widely-used assays like ELISA. “We used cells, rather than purified virus proteins, as the basis for our assay, which is closer to real physiology,” says lead author Vilja Pietiäinen of the Institute for Molecular Medicine Finland (FIMM) at the University of Helsinki. “Because everything is completely automated, we have high throughput, but we also get the digital images that can be shown to a virologist or a pathologist, without them having to go to a microscope. The results can even be checked on a mobile device. And we can count the number of infected cells, so we have the quantitative data as well as the visuals.”
During the early days of the pandemic, the research team was able to form quickly thanks to earlier international and local collaborations on virology, imaging and drug response studies, explains Pietiäinen. “At that point, we needed a high-throughput assay for antibody testing that would indicate if a person had a SARS-CoV-2 infection. Since then, there has been a lot of improvement on SARS-CoV-2 diagnosis, detection, and antibody response,” such as the widely familiar polymerase chain reaction (PCR) test or the antigen test (such as the nose swab) that directly measure the presence of the virus in the body. The test developed by Pietiäinen, Guckelsberger and colleagues, by contrast, measures antibodies, which tells us how the immune system is recognizing the virus and producing different types of antibodies against it.
Image: Minttu Polso
“When you only have a few samples, know very little about a disease or might not have access to a high-level biosafety lab, our pipeline can be really valuable,” says Guckelsberger, adding that it can be used anywhere regardless of location, sample preparation equipment or type of microscope. In fact, the pipeline is versatile to test on any germ. “We designed the test to be used for any emerging pathogen, increasing our readiness for future pandemics,” says Pietiäinen. “Certain components should be optimized for each new virus, but the beauty of the assay is that it can be used for different purposes. It’s already being used to study zoonotic viruses like the Puumala virus.” Other automated cell-based assays, followed by AI-guided image analysis methods, are being used in the research group to study the drug responses to SARS-CoV-2 as well as to identify drugs that can kill patient-derived cancer cells ex vivo.
Beyond publishing their work and contributing to a better understanding of the pandemic, Guckelsberger and Pietiäinen share a common insight that this project taught them. “When big questions come up in the world, we as scientists can’t work alone in silos. Experts from different fields, different universities and countries need to come together with a shared aim—in our case, data scientists, clinicians, computer scientists, biochemists,” says Pietiäinen.
“Working in a big team, which is not something we do often in computer science, was fascinating,” echoes Guckelsberger. “One big challenge was communicating from different perspectives of expertise, for example making sense of what is happening at both ends of the pipeline from wet lab procedures to parameters to data and images. At the same time, this was a fantastic learning experience, and one that I wish to have more of in the future.”
While they employed well-established machine learning for each component of the pipeline, Guckelsberger says making the connection between biologists and computer scientists was one of the real advances. Using technology to resolve biological questions was a big takeaway for Pietiäinen, too. “Combining microscopy with machine learning, not just for SARS-CoV-2, but to see personalized responses to drugs or to see the cellular phenotypes of rare genetic diseases, is powerful. A picture is worth a thousand words, that is also the case here.”